Can Gum Disease Ruin Your Dental Implants? Risks & Prevention Guide

You expect dental implants to last for many years. But if your gums are not healthy, you put that investment at risk. Gum disease can quietly damage the tissue and bone that hold your implant in place.
Yes, gum disease can ruin your dental implants if you do not treat it and keep it under control. Infection around the implant can lead to swelling, bone loss, and even implant failure. The good news is that you can prevent most of these problems with the right care.
You can protect your smile by understanding the risks of gum disease and dental implants, treating gum issues early, and keeping up with daily cleaning and dental visits. When you stay proactive, you give your implants the support they need to last.
Key Takeaways
- Healthy gums and strong bone are essential for long-lasting dental implants.
- An untreated gum infection can lead to bone loss and implant failure.
- Consistent home care and regular dental visits lower your risk of complications.
How Gum Disease Threatens Dental Implants
Gum disease can weaken the tissue and bone that support your dental implants. Infection, inflammation, and bone loss all raise the risk of implant failure and long-term problems.
The Link Between Gum Disease and Implant Failure
Gum disease is an infection that attacks the soft tissue and bone around your teeth. When it turns into periodontitis, it can also harm the area where your implant sits.
Dental implants need healthy gum tissue and a strong jawbone to stay secure. If bacteria remain under the gums, they can slow healing after implant surgery. This makes it harder for the implant to bond with your bone.
Research shows implants often succeed, but infections remain a common reason for problems over time. The article on the connection between dental implants and gum disease explains that untreated gum infections can threaten long-term results.
If you have active gum disease, your dentist will usually treat it before placing an implant. Skipping this step raises your risk of implant failure.
Peri-Implantitis: Infection Around Implants
Even after your implant heals, infection can still develop. This condition is called peri-implantitis.
Peri-implantitis affects the gum and bone around a dental implant. You may notice:
- Red or swollen gums
- Bleeding when brushing
- Bad taste or odor
- A loose implant
This infection acts much like periodontitis around natural teeth. Bacteria collect around the implant, irritate the tissue, and start breaking down bone.
If you ignore these signs, the damage can spread deeper into the jawbone. Early treatment can control the infection and protect implant stability. Regular cleanings and daily brushing and flossing lower your risk.
Implant Stability and Jawbone Loss
Your implant depends on osseointegration, which means the jawbone grows tightly around the implant post. Bone loss weakens this bond.
When gum disease destroys bone, it reduces the support under your implant. Less support means less implant stability. Over time, the implant can loosen.
Bone loss does not always cause pain at first. You may only notice slight movement or changes in how your bite feels.
If bone loss becomes severe, your dentist may need to remove the implant. In some cases, you may need a bone graft to rebuild the jawbone before placing a new implant.
Protecting your gums protects your jawbone. Healthy tissue and strong bone give your dental implants the best chance to last.
Worried that gum disease may be affecting your implants? Don't wait until you notice pain or movement, contact us today, as early treatment can save both your gums and your investment.
Understanding Gum Disease and Related Risks
Gum disease can slowly damage the tissue and bone that support your teeth and implants. When you understand how it starts and progresses, you can take clear steps to protect your gum health and lower your risk.
Stages: Gingivitis to Periodontitis
Gum disease, also called periodontal disease, starts with gingivitis. At this stage, your gums may look red or swollen. You might notice bleeding when you brush or floss.
Gingivitis affects only the soft tissue. The bone that supports your teeth and implants is still healthy. With good brushing, flossing, and professional cleanings, you can often reverse it.
If you ignore gingivitis, it can turn into periodontitis. This stage is more serious. The infection spreads deeper and begins to damage the bone under your gums.
As bone breaks down, teeth can loosen. Dental implants can also lose support. Bone loss makes it harder for an implant to stay stable over time.
How Plaque and Tartar Contribute
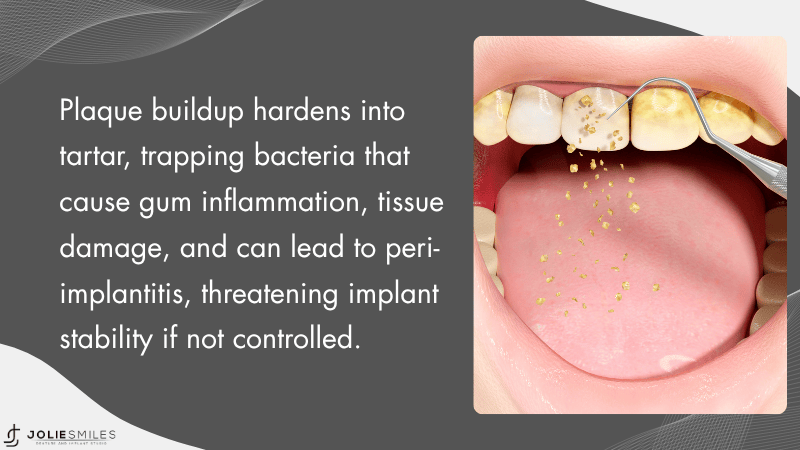
Plaque is a sticky film of bacteria that forms on your teeth every day. When you skip brushing and flossing, plaque builds up along the gumline.
If you do not remove plaque, it hardens into tartar. You cannot remove tartar at home. A dental professional must clean it off with special tools.
Plaque and tartar hold bacteria against your gums. This causes irritation and infection. Over time, the bacteria release toxins that damage soft tissue and bone.
If you already have implants, this buildup can lead to inflammation around the implant. A condition called peri-implantitis can develop, which is similar to periodontitis and can threaten implant stability.
Keeping plaque under control is one of the most direct ways you protect your gum health.
Signs You May Be at Risk
You may be at risk for gum disease if you notice:
- Gums that bleed when brushing
- Persistent bad breath
- Gum tenderness or swelling
- Gums pulling away from teeth
- Loose teeth or shifting bite
Smoking, diabetes, and poor oral hygiene also increase your risk. A history of periodontal disease makes future problems more likely.
Regular dental exams help catch small changes early. When you treat gingivitis or early periodontitis right away, you reduce the chance of bone loss and protect both your natural teeth and your dental implants.
Implant Candidacy: Evaluating and Restoring Gum Health
Your dentist must confirm that your gums and jawbone can support implant placement. You may still qualify with a history of gum disease, but you need careful evaluation and treatment first.
Assessing Implant Eligibility
Your provider starts by checking for active gum infection. Red, swollen, or bleeding gums often signal ongoing disease that can threaten implant eligibility.
They will measure gum pockets around your teeth and take X‑rays to review bone levels in your jawbone. Deep pockets and bone loss raise the risk of implant failure.
A review of your medical history also matters. Smoking, uncontrolled diabetes, and poor oral hygiene can lower healing ability and affect long‑term stability.
Many patients with past gum problems still qualify after proper care. As explained in this guide on dental implants and gum disease, healthy gums and stable bone are key before moving forward.
Your dentist will not place implants if disease remains active. Controlling infection comes first.
Treating Gum Disease Prior to Placement
You must complete gum disease treatment before implant placement. This step protects the jawbone and lowers the chance of infection around the implant.
Treatment often begins with scaling and root planing. This deep cleaning removes plaque and bacteria below the gum line.
If infection persists, your dentist may use antibiotics or recommend minor gum surgery. The goal is simple: stop inflammation and allow your tissue to heal.
Active periodontal disease increases the risk of peri‑implantitis, a serious infection that can destroy bone around implants. Many specialists stress that gum disease must be resolved before implant placement to reduce failure risk.
After treatment, you will return for follow‑up exams. Your provider checks that your gums look pink, firm, and stable before scheduling surgery.
Planning to get dental implants in Odessa, FL? Schedule your visit today to evaluate your gums and bone to ensure you're a candidate before moving forward.
Role of Bone Grafting and Jawbone Health
Healthy implants need strong bone. Gum disease can shrink your jawbone over time, which weakens support.
If X‑rays show bone loss, your dentist may suggest bone grafting. This procedure adds bone material to rebuild the area where the implant will sit.
Bone grafts can use your own bone, donor tissue, or synthetic material. Over several months, your body forms new bone that strengthens the site.
Patients with advanced bone loss often require grafting before they qualify. As outlined in this discussion of getting dental implants with gum disease, rebuilding bone support improves implant stability and long‑term success.
A strong jawbone structure provides the implant with a firm base. Without it, the implant may loosen or fail under normal biting pressure.
Protecting Implants: Daily Care and Professional Maintenance
Healthy implants depend on consistent at-home oral hygiene and routine care at your dental office. You need to control plaque every day and let your dentist monitor your gums and bone.
Oral Hygiene Practices for Implant Health
You must treat your implant like a natural tooth, even though it cannot get cavities. Plaque can still build up around the crown and gumline. That plaque can lead to infection and bone loss.
Brush twice a day with a soft toothbrush. Angle the bristles toward the gumline and clean all sides of the implant crown.
Floss daily to remove plaque between teeth and around the implant. If floss feels hard to use, try interdental brushes or floss made for implants.
Focus on these daily steps:
- Brush for two minutes
- Floss daily
- Rinse if your dentist recommends it
- Clean under bridges with special threaders if needed
Good home care lowers your risk of peri-implantitis, which is gum disease around implants. Many experts stress the need for strong daily habits in guides like this one on how to maintain healthy gums and teeth around your implants.
Importance of Regular Dental Checkups
Even strong oral hygiene at home is not enough on its own. You still need regular dental checkups so your dentist can check your gums and bone levels.
Most people with implants need dental checkups every 3 to 6 months. Your dentist will measure the pockets around the implant and look for bleeding or swelling.
At these visits, your dental team will:
- Check implant stability
- Review your brushing and flossing habits
- Take X-rays when needed
- Look for early signs of bone loss
Implants need healthy gums to last. Many providers explain the link between gum health and long-term success in articles such as the importance of gum health after dental implant treatment.
Regular dental checkups help catch small problems before they turn into implant failure.
Professional Cleanings and Deep Cleaning
Professional cleanings remove hardened plaque that brushing cannot remove. Your hygienist uses tools made for implants to avoid scratching the surface.
During professional cleanings, your dental team will clean above and below the gumline. This helps prevent inflammation around the implant.
If your dentist finds signs of infection, you may need a deep cleaning. This treatment, also called scaling and root planing, removes bacteria from deeper pockets around the implant.
A deep cleaning may include:
- Cleaning below the gumline
- Smoothing root surfaces
- Antibacterial rinses
Dental professionals outline these steps in detailed guides like this dental implant maintenance guide.
Professional cleanings and deep cleaning protect the bone that supports your implant. When you combine them with strong oral hygiene and regular dental checkups, you give your implants the best chance to stay stable for years.
Already have implants? Protect them with regular gum evaluations and professional cleanings designed specifically for implant patients like you.
Managing Risk Factors and Long-Term Success
You protect your implant success by controlling daily habits and treating gum problems early. Small actions now can prevent bone loss, infection, and costly repairs later.
Smoking and Other Risk Factors

Smoking is one of the biggest threats to dental implants. It reduces blood flow to your gums, slows healing, and makes infection more likely. Smokers often do not notice early signs of gum disease, which allows damage to grow without pain.
If you have a history of periodontal disease, you face a higher risk of implant problems. Bacteria that harmed your natural teeth can also infect the tissue around implants.
Other risk factors include:
- Poor brushing and flossing
- Skipping dental cleanings
- Uncontrolled diabetes
- Teeth grinding
- Weak bone support
Experts explain that active gum disease must be treated before implant placement because infection can cause failure, as noted in this guide on gum disease and dental implants.
Quitting smoking and managing health conditions greatly improve healing and long-term stability.
Preventing Peri-Implantitis
Peri-implantitis is an infection around a dental implant. It damages gum tissue and destroys supporting bone. Without treatment, it can loosen or ruin the implant.
Plaque buildup is the main cause. Your body reacts to bacteria the same way it would around a natural tooth. Inflammation begins, pockets form, and bone loss may follow.
According to this article on periodontal disease and its impact on dental implants, regular checkups and professional cleanings help detect problems early.
To lower your risk:
- Brush twice a day along the gum line
- Floss daily around the implant
- Use tools your dentist recommends, such as interdental brushes
- Keep routine dental visits every 3–6 months
Early treatment of gum inflammation protects bone and keeps your implant secure.
Maintaining Long-Term Oral Health
Dental implants can last many years, but they need steady care. Healthy gums are the foundation of long-term oral health.
You should treat your implant like a natural tooth. Clean it every day and never skip maintenance visits. Your dentist will measure pocket depths and check bone levels during exams.
Specialists stress that healthy gums play a direct role in implant stability, as explained in this review of the role of gum health in dental implant success.
Simple habits make a real difference:
- Keep plaque under control
- Address bleeding gums right away
- Replace worn night guards if you grind your teeth
- Follow your dentist’s maintenance schedule
When you stay consistent, you protect your investment and support lasting implant success.
Treatment Options After Complications
If your implant develops problems, quick treatment can protect your gums and bone. Dentists use targeted gum therapy, deep cleaning, medication, and other procedures to control infection and save the implant when possible.
Treating Peri-Implantitis and Gum Infection
Peri-implantitis is an infection that affects the gum and bone around your implant. It often causes bleeding, swelling, bad breath, and bone loss. If you ignore it, the implant can loosen.
Your dentist will start with deep cleaning around the implant surface. This form of gum therapy removes plaque and hardened buildup below the gum line. Special tools clean the implant without damaging it.
You may also need:
- Antibacterial rinses
- Local antibiotic medication placed under the gums
- Minor surgery to lift the gum and clean deeper areas
If bone loss has started, your dentist may place a bone graft to rebuild support. Early care gives you the best chance of keeping your implant stable.
Periodontal Treatment and Laser Therapy
If gum disease affects several teeth and implants, you may need full periodontal treatment. This often includes scaling and root planing, which removes bacteria from deep pockets around your teeth and implants.
Your dentist measures pocket depth to track infection. Healthy gums usually have shallow pockets. Deeper pockets signal an active disease that needs treatment.
Some offices use laser therapy as part of gum treatment. A dental laser targets infected tissue while leaving healthy tissue in place. This approach may reduce bleeding and swelling.
Laser therapy does not replace good home care. You still need to brush twice a day, floss daily, and attend regular cleanings every 3–6 months. Consistent care helps prevent the infection from returning.
Antibiotic Therapy and Root Canal Solutions
In some cases, your dentist may recommend antibiotic therapy to control bacterial infection. You might take oral antibiotics or receive medication placed directly around the implant. This step works best when combined with professional cleaning.
If pain comes from a nearby natural tooth rather than the implant, you may need a root canal. An infected tooth can spread bacteria to surrounding gum tissue and affect implant health. A root canal removes infected pulp inside the tooth and seals it to prevent further spread.
Your dentist will use X-rays and an exam to identify the true source of infection. Treating the right problem protects both your natural teeth and your implants.
Your implants depend on healthy gums, period. If you're noticing bleeding, swelling, or changes in how your implant feels, contact Jolie Smiles in Odessa, FL, right away.
Frequently Asked Questions
Gum disease can weaken bone, cause gum recession, and raise the risk of infection around implants. You can still qualify for treatment in many cases, but you may need gum therapy or bone support first.
Are dental implants an option for patients with receding gums?
Yes, but you need enough healthy bone and gum tissue to support the implant. Receding gums often point to past or active gum disease, so your dentist will check for infection and bone loss first.
If you have mild recession, a gum graft can rebuild lost tissue. This helps protect the implant and improve appearance.
Your dentist may also review how gum disease affects dental implants before moving forward.
Is it possible to get dental implants if you suffer from severe gum disease?
You usually need to treat severe gum disease before you get implants. Deep cleaning, medication, or gum surgery can control infection and reduce inflammation.
In some cases, you may also need a bone graft if gum disease has damaged your jawbone. After your gums become stable and healthy, you can move ahead with implant placement.
Dentists often explain that gum disease needs treatment before implant placement to improve healing and long-term success.
How does gum disease affect the success of All-on-4 dental implants?
All-on-4 implants rely on strong bone in specific areas of your jaw. If gum disease has reduced bone volume, it can limit where implants can anchor safely.
Active infection also raises your risk of peri-implantitis, an inflammation around implants. This condition can lead to bone loss and implant failure if you do not treat it early.
Your dentist will check bone levels with imaging before recommending this option.
What are the alternatives to dentures for those with gum disease?
Implant-supported bridges can replace several teeth without a full denture. You must still control gum disease before placing implants.
In some cases, dentists combine gum therapy with partial implants to improve stability. Many providers note that dental implants for patients with gum disease remain possible with careful planning and follow-up care.
If implants are not an option, a well-fitted partial denture may still restore function while you manage your gum health.
At what point is it considered too late to reverse the effects of gum disease for implant candidacy?
It is rarely “too late,” but advanced bone loss makes treatment more complex. If you have lost a large amount of jawbone, you may need bone grafting before implants.
Uncontrolled diabetes, heavy smoking, or untreated infection can also delay or prevent implant placement. Once your dentist controls infection and restores enough bone support, you may qualify again.
Early treatment gives you more options and lowers your risk of future problems.
How common is infection in dental implants and how can it be prevented?
Dental implants have high long-term success rates, but infections like peri-implantitis can still occur. This condition affects the gum and bone around the implant.
You can lower your risk by brushing twice a day, flossing daily, and keeping regular dental visits. Many experts stress that peri-implantitis can lead to implant failure if not treated.
Avoid smoking, manage health conditions, and follow your dentist’s cleaning schedule to protect your investment.
