When Do You Need a Dental Implant Restoration Instead of Replacement?

Dental implants can last for many years, but the visible parts attached to them may need attention over time. A crown sitting on top of an implant might chip, wear down, or become discolored while the implant post in your jawbone remains perfectly healthy.
Understanding when you need a restoration versus a full replacement can save you time and money.
You need a dental implant restoration when the implant post itself is still secure and healthy in your jawbone, but the crown, bridge, or denture attached to it needs repair or replacement.
Restoring a dental implant involves fixing the visible part without touching the implant post below. This happens more often than full replacements because the titanium post typically outlasts the restoration attached to it.
Knowing the difference between these two options helps you make better choices about your dental care. Your dentist will check both the implant post and the restoration to decide which approach keeps your smile healthy and functional.
Key Takeaways
- Dental implant restoration fixes or replaces the crown, bridge, or denture while keeping the original implant post intact
- You need restoration when your implant post stays secure but the visible tooth shows wear, damage, or looseness
- Regular dental checkups help catch problems early so you can restore implants before needing full replacement
Understanding Dental Implants and Implant Restorations
A dental implant consists of multiple parts working together to replace a missing tooth. Knowing the difference between fixing the visible crown and replacing the entire implant system helps you make better decisions about your dental care.
What Is a Dental Implant?
A dental implant is a titanium post that gets surgically placed into your jawbone to act as an artificial tooth root. The implant post fuses with your bone over several months through a process called osseointegration.
This titanium post provides a stable foundation for replacement teeth. Unlike dentures or bridges that sit on top of your gums, dental implants are surgically inserted to create permanent support.
The implant becomes part of your jaw structure. Once healed, it can support crowns, bridges, or dentures just like natural tooth roots support your natural teeth.
How Implant Restorations Differ from Replacements
Implant restoration replaces or repairs the visible portion of your dental implant while keeping the original implant post in your jawbone. An implant replacement means removing the entire titanium post and starting over with a new implant.
You need restoration when your dental crown becomes worn, cracked, or discolored. The implant post stays in place because it remains healthy and secure.
Replacement becomes necessary when the implant post itself fails. This happens if the implant doesn't fuse properly with your bone or if you develop an infection around the post.
Restoration costs less and takes less time than full replacement. You avoid additional surgery since your jawbone and implant post don't need intervention.
Components of a Dental Implant System
A complete dental implant system has three main parts: the implant post, the implant abutment, and the final restoration.
The implant post sits inside your jawbone and acts as the root. The abutment connects to the top of the implant post and sticks up through your gum tissue. The final restoration is the visible dental crown, bridge, or denture that attaches to the abutment.
Each component serves a specific purpose:
- Implant post: Provides stability and preserves bone structure
- Abutment: Creates a secure connection point between the implant and crown
- Crown: Restores appearance and chewing function
When you need a dental implant restoration, your dentist typically replaces only the crown or abutment. The implant-supported crown might need updating after years of use, but the implant post can last for decades with proper care.
When Is Dental Implant Restoration Needed?
Your dental implant can last for decades, but the crown, bridge, or denture attached to it may need attention over time. Knowing when to seek restoration helps you maintain your smile and avoid more serious problems.
Signs Your Implant Restoration Needs Attention
You should watch for several warning signs that indicate your implant-supported crown needs care. A loose crown is one of the most common issues you might notice when eating or brushing your teeth.
Pain or discomfort around your implant area often means something is wrong. You might also see visible cracks or chips in your crown or bridge. Changes in your bite or difficulty chewing are red flags that shouldn't be ignored.
Gum inflammation or bleeding around the implant site needs immediate attention. If you notice your restoration looks different in color compared to your other teeth, it may be time for a replacement. Any clicking or movement when you touch the crown with your tongue is a clear sign to call your dentist.
Common Causes: Wear, Damage, and Gum Issues
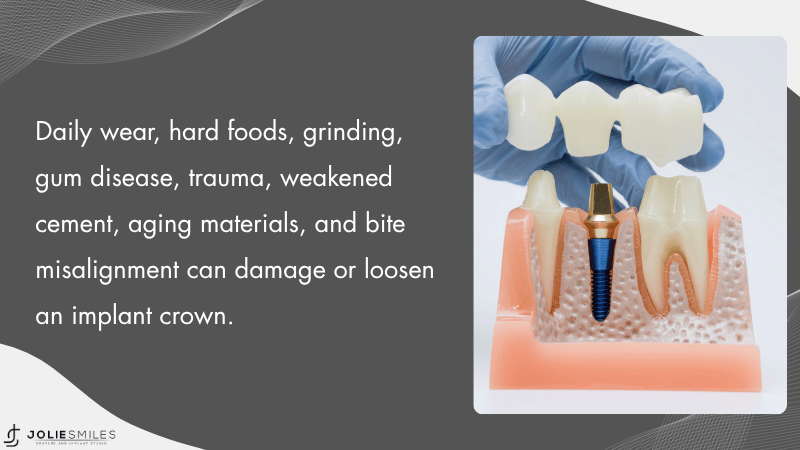
Your implant restoration faces daily stress from chewing, grinding, and normal wear. The damaged implant crown often results from biting hard foods like ice or candy. Teeth grinding at night can wear down or crack your crown over time.
Gum disease around your dental implant can compromise the restoration's stability. Poor oral hygiene allows bacteria to build up, leading to inflammation and bone loss. Accidents or facial trauma can chip or break your crown even if the implant itself stays secure.
The cement holding your crown to the abutment can weaken after several years. Normal aging of dental materials means your crown may discolor or lose its shine. Some people develop issues with their dental implant due to bite misalignment that puts extra pressure on one area.
Types of Restorations: Crowns, Bridges, and Dentures
Single crowns are the most common type of dental implant restoration for one missing tooth. Your dentist attaches a custom-made crown to the abutment on top of your implant. This option works well when you have healthy teeth on both sides.
Implant-supported bridges replace multiple missing teeth using two or more implants. The bridge attaches to implants on either end, eliminating the need to alter your healthy teeth. This restoration is more stable than traditional bridges that rely on adjacent teeth.
Implant-supported dentures provide a secure solution for replacing an entire arch of teeth. These dentures snap onto or screw into several strategically placed dental implants. They offer better chewing function and comfort compared to traditional removable dentures.
Book a consultation today to find out if your implant needs restoration or replacement.
When Is Dental Implant Replacement Necessary?
A failing implant shows clear warning signs that require professional attention. When the metal post becomes loose or the bone around it deteriorates, full replacement becomes the only solution to protect your oral health.
Recognizing Implant Failure
Your body gives you signals when something goes wrong with your implant. Pain that persists weeks or months after your initial healing period often indicates a problem with the implant itself. A healthy dental implant should feel stable and comfortable, just like your natural teeth.
You might notice your implant moving when you chew or touch it with your tongue. This wobbling means the connection between the titanium post and your jawbone has weakened. Swollen or bleeding gums around the implant point to infection, which can spread quickly if left untreated.
Bad breath or an unusual taste in your mouth that won't go away also suggests bacterial growth around the implant site. These symptoms mean you need to visit your dentist right away to prevent further damage.
Severe Structural or Biological Issues
Problems with osseointegration are among the most common reasons you might need dental implant replacement. This process involves the titanium post fusing with your jawbone to create a stable foundation. When this fusion fails, no amount of repair work will fix the problem.
Significant bone loss around your implant makes it impossible for the post to stay secure. Your jawbone may lack the strength needed to support the implant properly, especially if you have untreated gum disease or certain health conditions. In these cases, you'll need the failed implant removed before any new restoration can begin.
Some people require bone grafting to rebuild the jawbone before a new implant can be placed. Your dentist will evaluate whether your bone structure can support a replacement or if additional procedures are necessary first.
Risks and Considerations for Replacement
Dental implant replacement involves removing the failed post and allowing your jaw to heal before placing a new one. This process takes longer than your original implant surgery because damaged tissue needs time to recover. Your healing period might last several months, depending on how much bone loss occurred.
Infection risk increases with each surgical procedure, so your dentist will carefully evaluate your oral health before proceeding. You may need antibiotics or special cleaning treatments to eliminate bacteria before replacement can happen.
The success rate for replacement implants depends on addressing what caused the original failure. If smoking, poor oral hygiene, or uncontrolled diabetes contributed to the problem, you'll need to make changes to protect your new implant.
The Dental Implant Restoration Process
The restoration process involves careful assessment of your existing implant, selection of appropriate materials, and coordination between specialized dental professionals to ensure a successful outcome.

Initial Evaluation and Diagnosis
Your dentist begins with a comprehensive examination to determine the condition of your existing implant and surrounding tissues. This evaluation includes X-rays or digital imaging to assess bone density, gum health, and the stability of the implant post.
During this visit, your dentist checks for signs of wear, damage, or loosening in your current restoration. They measure the fit of your crown, bridge, or denture to identify any gaps or misalignment. The dental implant restoration process requires precise measurements to ensure your new restoration fits properly.
Your dentist also evaluates your bite pattern and jaw alignment. This helps them understand how forces are distributed across your teeth when you chew. Based on these findings, they create a customized treatment plan that addresses your specific needs.
Restoration Techniques and Materials
Your restoration is fabricated using durable materials like porcelain or zirconia that match your natural teeth. These materials are selected based on the location of your implant and the amount of chewing force it will endure.
The dental implant procedure for restoration involves either replacing just the crown portion or adjusting the entire prosthetic. Single tooth restorations use custom-made crowns attached to the abutment. Multiple tooth restorations may require bridges or partial dentures supported by several implants.
Your dentist takes impressions or digital scans of your mouth to create a restoration that fits precisely. The new crown or prosthetic is designed to match the color, shape, and size of your surrounding teeth. Once ready, your restoration is securely attached to the implant post, and your dentist checks your bite to ensure proper alignment.
Role of the Dental Implant Specialist
A prosthodontist specializes in designing and placing dental restorations on implants. They focus on creating prosthetics that restore both function and appearance. Your prosthodontist works closely with dental labs to ensure your restoration meets exact specifications.
An oral surgeon or periodontist may be involved if you need adjustments to the implant placement or surrounding tissues. These specialists handle complications like gum recession or bone loss that can affect implant stability. They ensure the foundation supporting your restoration remains healthy and strong.
Your specialist monitors your healing progress and makes adjustments as needed. They provide guidance on proper care techniques to extend the life of your restoration.
Long-Term Care and Maintenance Tips
Taking care of your dental implants requires daily attention and regular professional support. Proper cleaning techniques, the right tools, and healthy habits protect both the implant and surrounding gum tissue from damage.

Daily Oral Hygiene Routines
Brushing your teeth twice daily keeps your dental implants clean and free from harmful bacteria. You should use a soft-bristled toothbrush with non-abrasive toothpaste to avoid scratching the implant surface or damaging your dental crown.
Flossing around your implants removes food particles and plaque that brushing alone cannot reach. Regular flossing prevents buildup that can lead to gum recession and other complications. You need to be gentle when cleaning around the implant to protect the delicate gum tissue.
Pay special attention to the areas where your implant meets the gums. This zone collects bacteria easily and requires thorough cleaning. Making these habits part of your daily routine helps maintain your oral health and extends the life of your implants.
Tools for Implant Maintenance
An interdental brush works well for cleaning hard-to-reach spaces between your implants and natural teeth. These small brushes come in different sizes to fit various gaps. Water flossers provide another effective option for removing debris around the implant without irritating sensitive gums.
You might also benefit from using antimicrobial mouth rinse to reduce bacteria levels in your mouth. Specialized cleaning tools designed specifically for implants can make your daily care routine more effective. Avoid using metal instruments or abrasive materials that could scratch or damage your implant restoration.
Your dentist can recommend the best combination of tools based on your specific needs. Investing in quality cleaning products protects your implants and helps them last longer.
Dental Checkups and Professional Cleanings
You should visit your dentist every three to six months for professional cleanings and examinations. These appointments allow your dentist to check the stability of your implants and spot potential problems early. Professional evaluations include checking implant stability and examining the surrounding bone and tissue.
During cleanings, dental professionals use specialized instruments designed for implants. They remove plaque and tartar that build up over time, even with excellent home care. Regular checkups help prevent complications that could require more extensive treatment later.
Your dentist will also assess whether your implant crown shows signs of wear or damage. Early detection of issues makes restoration simpler and less costly than waiting until problems become severe.
Lifestyle Habits to Prolong Implant Longevity
Avoiding hard foods like ice, hard candy, and popcorn kernels protects your dental crown from cracks and chips. You should never use your teeth as tools to open packages or bottles. These habits place unnecessary stress on your implants.
If you grind your teeth at night, wearing a protective mouthguard prevents damage to both your implants and natural teeth. Smoking slows healing and increases the risk of implant failure, so quitting improves your chances of long-term success.
Eating a balanced diet supports your overall oral health and helps maintain strong bone structure around your implants. Good oral hygiene combined with healthy habits gives your implants the best chance of lasting decades.
Benefits of Timely Restoration Versus Replacement
Acting quickly to restore a dental implant rather than replacing it entirely protects the bone structure around your implant and saves you both time and money. The right approach at the right time keeps your smile functional and attractive while avoiding unnecessary procedures.
Preserving Jawbone and Oral Health
When you address implant issues through restoration instead of replacement, you protect the osseointegration that has already occurred between your implant and jawbone. This bond takes months to develop after initial placement. Replacing an entire implant means removing it from your jawbone and starting this process over again.
Your jawbone stays healthier when the implant post remains in place. Removing an implant can damage surrounding bone tissue and require bone grafting before a new implant can be placed. Restorative procedures that focus on fixing the crown or abutment leave your jawbone structure intact.
The tissue around your implant also benefits from restoration over replacement. Your gums have adapted to the implant shape and position. Keeping the existing post means less disruption to your soft tissues and faster healing times.
Reducing Cost and Invasiveness
Restoration costs significantly less than full replacement because you only pay for the damaged component. A new crown or bridge attached to your existing implant typically costs 50-70% less than removing and replacing the entire implant system.
The procedure itself is much simpler when you choose restoration. You avoid surgery, anesthesia, and the extended healing period that comes with implant removal and placement. Most restoration procedures take one or two appointments instead of several months.
Your recovery time is minimal with restoration. You can usually return to normal eating and activities within a few days rather than waiting months for a new implant to integrate with your bone.
Improving Confidence and Daily Function
A timely restoration gets your smile back to normal quickly so you can eat, speak, and interact without worry. Worn or damaged crowns affect how you look and feel during conversations and meals.
Your bite alignment stays correct when you restore rather than remove an implant. The existing implant is already positioned properly in your jaw. Replacing it risks slight changes in positioning that could affect how your teeth come together.
You maintain the natural appearance you've grown accustomed to with restoration. Modern materials match your existing teeth in color and shape, so no one will notice the difference.
Frequently Asked Questions
Many people wonder about the warning signs that signal a problem with their implant and whether fixing the existing one makes more sense than starting over. Understanding what causes implant issues and how long these tooth replacements typically last helps you make better decisions about your dental care.
What signs indicate that I might need a dental implant restoration?
You might notice your implant crown feels loose when you touch it with your tongue or while eating. This movement suggests the restoration has come detached from the implant post.
Pain or discomfort around the implant area can signal problems with the restoration or surrounding tissues. You should pay attention if the area becomes tender when you chew.
Visible damage like chips, cracks, or discoloration on your implant crown means you need restoration work. The crown may also look different from your natural teeth if it has worn down over time.
Gum tissue pulling away from the implant or bleeding around it indicates potential complications. These common issues that lead to dental implant restoration require professional evaluation.
How can I tell if a repair is possible, or do I need a complete implant replacement?
Your dentist will take X-rays to check if the implant post remains stable in your jawbone. A secure post usually means you only need to replace the crown or other visible parts.
Bone loss around the implant or a loose post suggests you might need complete replacement. Your dentist can measure bone density and implant stability during your exam.
The condition of your gums also affects whether repair works for your situation. Healthy gum tissue supports restoration, while severe gum disease may require more extensive treatment.
What are common issues that lead to the need for dental implant restoration?
Worn or damaged crowns represent one of the most frequent problems with dental implants. Daily wear from chewing can cause fractures or surface damage over many years.
Loose restorations happen when the connection between the crown and implant weakens. You might feel the crown shift slightly or notice it moves when you eat certain foods.
Gum recession or bone loss around the implant can create gaps that affect stability. These changes in your mouth structure may happen gradually as you age or due to poor oral hygiene.
Some people need restoration for cosmetic reasons when their implant crown no longer matches their other teeth. This happens as natural teeth change color while the crown stays the same shade.
Can a damaged dental implant be fixed, or is replacement my only option?
Many damaged implants can be fixed without removing the post from your jawbone. Your dentist can replace just the crown, bridge, or denture attached to the implant.
The implant post itself rarely needs replacement if it remains firmly anchored in bone. Most restoration work focuses on the visible parts that experience daily wear.
Complete replacement becomes necessary only when the post fails or bone loss makes the implant unstable. Your dentist will recommend this option if repair cannot restore proper function.
What maintenance does a dental implant typically require to avoid restoration or replacement?
You need to brush around your implant twice daily with a soft-bristled toothbrush. Use gentle circular motions to clean where the crown meets your gum line.
Flossing or using interdental brushes removes food particles that regular brushing misses. Water flossers work well for cleaning hard-to-reach areas around implants.
Schedule professional cleanings and checkups at least twice per year. Your dentist can spot early signs of problems before they require major restoration work.
Avoid chewing hard foods like ice or using your teeth to open packages. These habits put unnecessary stress on your implant restoration.
How long do dental implants last before they need to be restored or replaced?
The implant post can last several decades or even a lifetime with proper care. Most people never need to replace the metal post placed in their jawbone.
Implant crowns typically last 10 to 15 years before needing replacement. The crown experiences more wear than the post since it handles all the chewing forces.
Your daily habits affect how long your implant restoration lasts. People who grind their teeth or chew hard foods may need restoration sooner than those with gentler habits.
Regular dental visits help extend the life of your implant by catching small problems early. Routine checkups and professional cleanings protect both the implant and surrounding tissues.
